Michel Zaffran has been Director of Polio Eradication at the World Health Organization since 2015. Due to retire later this year, Michel spoke with Rotary Editor, Dave King.
What has been the impact of COVID-19 on the Global Polio Eradication Initiative (GPEI)?
The impact of COVID-19 on the world has, of course, been significant, and so it also has been on the global polio eradication effort. Given that, operationally, polio vaccination campaigns are close-contact activities, they were deemed incompatible with the current physical distancing recommendations associated with the COVID-19 response efforts. As such, in March we had to take the very difficult decision to temporarily delay immunisation campaigns. The overriding priority was to ensure the health and safety of health workers, as well as communities.
Polio campaigns could have increased the risk of further spread of COVID-19, and thereby put at risk the children being vaccinated, those vaccinating and indeed those populations beyond. From a public health point of view, it was the only recommendation to make under this new reality.
Campaigns are resuming, with increased security measures for health workers and communities, which is good news, but unfortunately more children are left vulnerable to diseases such as polio. We are anticipating an increase in polio cases.

Dr Michel Zaffran has been Director of the World Health Organization’s Global Polio Eradication Initiative since 2015 and is set to retire this year.
How has the infrastructure of the GPEI been able to help with the fight against COVID-19?
In many countries, polio assets (personnel, logistics, operations) are uniquely positioned to assist national health systems to respond to the pandemic and ensure the crisis is dealt with as rapidly and effectively as possible. In many countries this is already the case and our infrastructure is already heavily and actively involved in the response.
This has always been the ‘Plus’ in ‘PolioPlus’, in other words the infrastructure built up to eradicate polio regularly helps respond to other disease outbreaks or humanitarian disasters.
It is therefore doubly important to continue to invest in PolioPlus: not just to help eradicate polio, but indeed to ensure that this infrastructure can continue to support other health emergencies, such as it is currently doing with COVID-19, for example by supporting contact tracing, educating communities on hygiene measures and physical distancing measures, and using the polio laboratory infrastructure for specimen analysis.
With the threat from polio greater in the autumn and winter months, what plans will be put in place to face this fresh challenge?
Polio is indeed a seasonal disease, and we know that the second half of the year marks the ‘high season’ for poliovirus transmission (usually associated with an increase in rains in tropical climate settings). This means that children are more exposed to poliovirus than during the ‘low season’ for polio, in the first half of the year.
The overriding urgent task we face is now that polio campaigns are resuming is to rapidly rebuild immunity for children and communities at highest risk.”
Given the impact of COVID-19 and a decline in immunity rates, we unfortunately anticipate an increase in cases, and possibly also international spread of the disease.
So the overriding urgent task we face is now that polio campaigns are resuming after their temporary pause, to rapidly rebuild immunity for children and communities at highest risk.
That is our overriding priority over the coming months, and this process has already started with emergency vaccination campaigns resuming in known infected and high-risk areas.
What is the current state of play in Pakistan and Afghanistan? How big a set-back was COVID-19 to the polio eradication programme?
Polio eradication at its core is relatively straight-forward, in the sense that if you vaccinate enough children in a given area, poliovirus has nowhere to hide and dies out. Where it becomes complicated is when children are missed, and this then allows the virus to continue to circulate. Efforts conducted thus far have allowed a country like Pakistan to reduce the annual burden of cases from 30,000 twenty years ago, to less than 150 last year, a tremendous achievement by any other measure of progress. But not if you are trying to eradicate a disease.
If you are trying to eradicate a disease, there is virtually no room for error. The reasons why some pockets of children remain under-or unvaccinated in parts of Pakistan and Afghanistan vary from area to area, and include such factors as large-scale population movements, inadequate infrastructure, poor oversight and lack of management, insecurity, community resistance, lack of trust triggered by misinformation or other factors.

Michel Zaffran at the Karachi Clinic in Pakistan
What both countries are now doing is analysing area by area what the real reason is for missing children, and then putting in place area-specific operational plans to overcome those reasons.
It is the same approach which was implemented in both India and Nigeria, when they launched their “final assault” that led to success, and we have extremely high engagement of both governments and virtually all sectors of civil society.
Our biggest challenge now, however, is the impact of the COVID-19 pandemic and the temporary forced pause in activities it had forced on the programme.
But in the interim, we had been putting everything in place so that – once the campaigns resumed – we would be able to move more rapidly and efficiently, even in the context of Covid, and that is now beginning to happen which is encouraging.
Nigeria and the African continent were declared polio-free in August by the World Health Organization. How significant a step is this?
Africa has achieved an historic public health success: the certification of the eradication of wild polioviruses (WPV), by the African Regional Certification Commission (ARCC). This independent ‘stamp of approval’ verifies that WPV is gone from Africa, which was celebrated on August 25th.
This success stands in stark contrast to 1996, a year when WPV paralysed more than 75,000 of our children across every country on the continent. It was also the year when Nelson Mandela, together with Rotary International, issued a stark call to action, to everyone. His challenge rang out loud and strong: Kick Polio Out of Africa! This success is a clear example of what can be achieved, when all these levels unite towards a common goal, and indeed, already the polio effort on the continent is helping to address other urgent public health challenges.
Africa has achieved an historic public health success: the certification of the eradication of wild polioviruses.”
But this success would be only half the story. In fact, polio eradication in Africa can today best be described as ‘an unfinished success story’. To finish it, the increasing threat of circulating vaccine-derived poliovirus (cVDPV) outbreaks on the continent must also be addressed. For even though they are not WPV and are such rare strains which can emerge in areas of low population immunity, they can also paralyse children. New approaches, including a new vaccine which can battle such strains more effectively, are available, and it is critical that these new strategies and tools are fully utilised to ensure children are fully protected against all strains of poliovirus.
While the focus of the polio eradication programme has been on Pakistan, Afghanistan and Nigeria, what is happening in the rest of the world? What incidents are you receiving reports of?
In 1985, when Rotary International launched its PolioPlus programme, wild poliovirus paralysed every single year, more than 350,000 children, in more than 125 endemic countries.
Today, the wild poliovirus remains endemic in only two countries to: Pakistan and Afghanistan. Africa has not detected any wild poliovirus since September 2016, and was certified as free of such strains on August 25th. The disease has been reduced by 99%, more than 18 million people are today walking who would otherwise have been paralysed, and more than 1.5 million lives have been saved. All of this is thanks to the tireless efforts of Rotary and Rotarians worldwide, to mobilise funds, to engage communities, to advocate with donor governments, to ensure parents are convinced of the need for vaccination.
In 1985, when Rotary International launched its PolioPlus programme, wild poliovirus paralysed every single year, more than 350,000 children, in more than 125 endemic countries.”
But 99% is not good enough in an eradication effort. Eradicating a disease is extremely difficult, which is why it has only been achieved once so far (with the eradication of smallpox in 1980). Unless we eradicate it completely in these remaining areas of Pakistan and Afghanistan, we run the risk that the disease will make a global resurgence. That is the nature of an eradication effort: one either eradicates, or one does not. There is no in between. Just in August, we have received news of outbreaks in both Yemen and Sudan. Such outbreaks will continue to occur unless we achieve eradication.
But the good news is: we have all the tools and tactics available to us to succeed even by 2023, in these last two countries.
The extraordinary accomplishments of polio eradication in India (last case in 2011) and in Africa are proof that it can and will be done. Success however will depend on ensuring the tools and tactics are fully financed and fully implemented. If that happens, success will follow.
The GPEI End Game Strategy sets out clear aims by 2023. Bearing in mind the impact of COVID-19, do you think this is still achievable?
Yes, absolutely, but success will depend on fully implementing the tools and tactics to achieve success. The polio programme has a long history of adapting to new challenges, be it operating in insecure environments, overcoming access issues, reaching children amidst large-scale population movements, etc. COVID-19 is yet another challenge, but operationally we are already addressing this, adapting our approaches to this new reality. The key is fully operationalising what we know works and also keeping a flexible approach.
What is happening behind the scenes at the World Health Organization which might help accelerate the End Game Strategy (e.g. vaccines)?
The polio programme is constantly adapting its approaches, and tools and tactics, given the realities on the ground: operational, political, societal, epidemiological and virological. Our aim is to ensure that we have the most relevant, tailored tools and tactics to achieve the biggest impact.
As part of this, we are in the process of developing a next-generation oral polio vaccine, novel OPV type 2, as an additional vaccine tool in our global arsenal against this disease. We hope to be able to deploy it on a large scale later this year. It means that countries at their disposal have a variety of different polio vaccines and formulations, to be used based on a prevailing epidemiology in their area. This allows countries to apply the most relevant vaccine or vaccines, to ensure children are protected in the most effective and rapid manner possible.
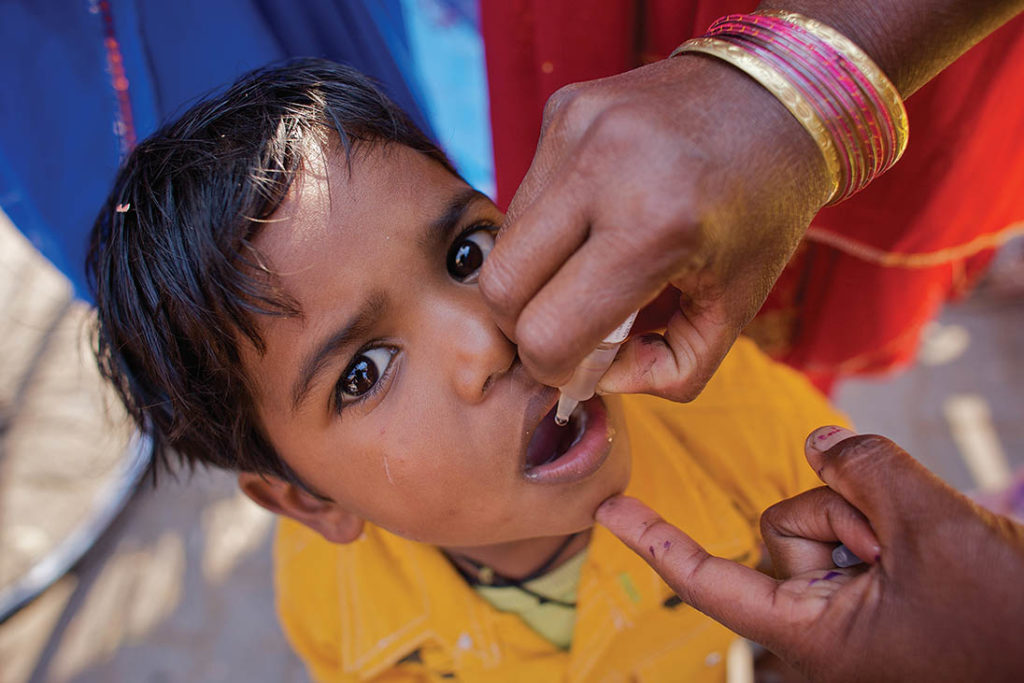
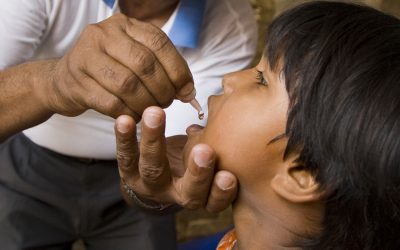
Polio is a disease which mainly affects children under the age of 5 and can cause paralysis and even death.
Do you still believe that polio will be fully eradicated in your lifetime – and why?
Not only in my lifetime, but actually over the next several years. Perhaps COVID1-9 gave us the final impetus to achieve success, because it has taught us a number of crucial lessons. For one: it reminded us how much we know about polio. The world today is trying to analyse how COVID-19 transmits, how widely it is spread, how best to combat it, which measures are effective and necessary, which are counterproductive. There are many medical questions left. For polio: we have all these answers.
We know how and where it spreads, and we know exactly what we need to do to stop it. We have all the technical tools and the knowledge. It is a question of implementing now what we know. And I believe countries have realised how dangerous infectious diseases are. How easily they spread across the world.
The world today is trying to analyse how COVID-19 transmits, how widely it is spread, how best to combat it, which measures are effective and necessary, which are counterproductive. There are many medical questions left. For polio: we have all these answers.”
And that when we do have effective measures, as we do against polio, we must fully implement them. It is literally a global public good. But the reality is also that we will not succeed without Rotary and Rotarians. Rotarians are the moral authority in this fight, leading with their personal engagement and resources. Rotarians must now redouble their efforts, to use that moral authority to hold governments accountable to finishing the job of polio eradication. Together, I am absolutely convinced that we will achieve a lasting success.
You are planning to retire from the World Health Organization this autumn. How will you reflect on your time in the fight against polio?
I have spent my entire career working in immunisation. Immunisations are one of the most effective public health and development interventions, any way one looks at it. Having been involved in the effort to eradicate polio has been an honour and privilege. When Rotary launched its PolioPlus effort in 1985, the concept was very simple: every child has a right to be vaccinated and protected from polio, no matter where they live, whether it be in Switzerland or the UK or Ireland, or in Somalia or the Democratic Republic of Congo. And that is what this programme has strived to do. To reach and vaccinate every single child.
It is literally the definition of equity. And this is probably the single most inspiring aspect about this programme and it has been simply inspirational to have been allowed to be a part of it. I will be retiring indeed from WHO at the end of the year, I will however remain a Rotarian and I will continue to advocate for PolioPlus.